Lung Asymmetry Explained: Why Your Lungs Aren’t Mirror Images (and Why It Matters)
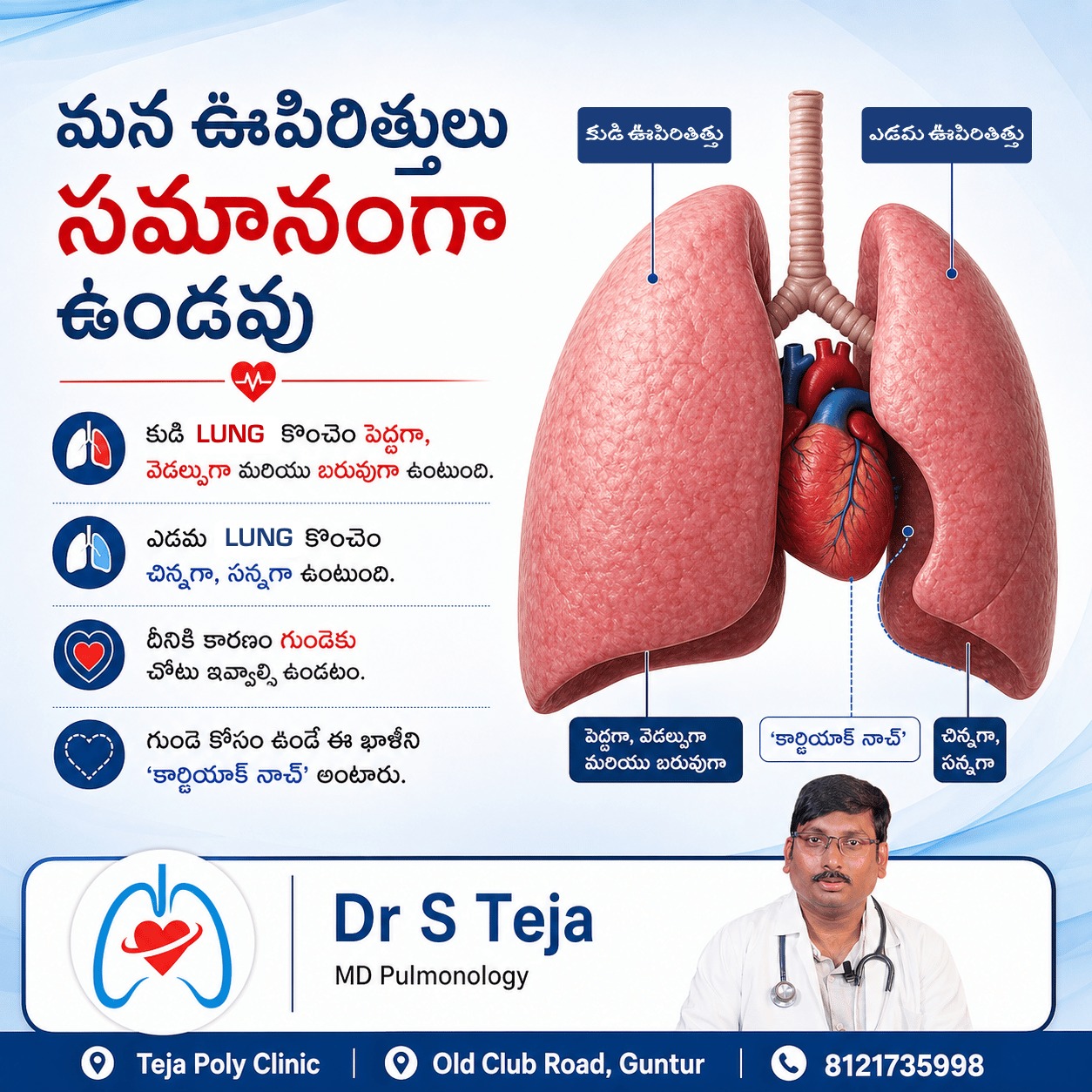
Lung Asymmetry Explained: Why Your Lungs Aren’t Mirror Images (and Why It Matters) The Uneven Design of Breathing When people imagine the human body, they often picture perfect symmetry. However, lung asymmetry explained reveals a different story. Your lungs are not identical mirror images—and that’s by design. The reason lies in the position of your heart. Located slightly to the left side of your chest, the heart occupies space that the left lung would otherwise fill. To compensate, your lungs have evolved with structural differences that prioritize function over symmetry. The Right Lung: The Heavy Lifter The right lung is larger and more robust, designed to handle a greater share of respiratory workload. Structure: It consists of three lobes—superior, middle, and inferior. Shape: Shorter but wider due to the upward push from the liver below. Function: Has greater volume and capacity, making it more efficient in gas exchange. Because of its size and structure, the right lung plays a dominant role in breathing efficiency. This is a key point in understanding lung asymmetry explained in clinical practice. The Left Lung: Making Room for the Heart The left lung adapts to accommodate the heart’s position. Structure: Contains only two lobes—superior and inferior. Cardiac Notch: A unique indentation that creates space for the heart. Shape: Narrower and slightly longer compared to the right lung. Although smaller, the left lung is equally vital. Its design ensures that both the respiratory and cardiovascular systems function harmoniously. When Nature Deviates: Structural Anomalies While this asymmetry is normal, some individuals are born with variations. A Pulmonologist in Guntur often evaluates these anomalies to determine whether they are harmless or clinically significant. 1. The Azygos Lobe An extra lobe can form in the right lung due to abnormal positioning of the azygos vein during development. Impact: Usually harmless but may be misinterpreted as a lung lesion in imaging. Clinical Note: Can complicate surgeries or confuse diagnoses. 2. Pulmonary Hypoplasia This condition occurs when one or both lungs do not fully develop. Impact: Reduced lung capacity and impaired oxygen exchange. Associated Conditions: Respiratory distress and pulmonary hypertension. Early diagnosis is critical, and consultation with a Pulmonologist in Guntur can help manage symptoms effectively. 3. Situs Inversus (Mirror Image Organs) In rare cases, the body’s organs are reversed. The heart is on the right side (dextrocardia). Lung lobes are also reversed. Associated Syndrome: Kartagener’s Syndrome Impact: Chronic sinus infections, bronchiectasis, and recurring lung infections due to impaired cilia function. 4. Accessory Lobes and Sequestrations Some individuals develop extra lung tissue that lacks proper airway or blood supply connections. Condition: Bronchopulmonary sequestration. Impact: Increased risk of recurrent infections or cyst formation. Clinical Comparison: Right vs Left Lung Feature Right Lung Left Lung Potential Issue Lobes 3 2 Accessory lobes Bronchus Wider, vertical Narrower, horizontal Aspiration risk (right side) Landmark Horizontal fissure Cardiac notch Situs inversus One important clinical takeaway is that foreign objects are more likely to enter the right lung due to its wider and more vertical bronchus. Why Understanding Lung Asymmetry Matters Understanding lung asymmetry explained is crucial for both diagnosis and treatment. Accurate Diagnosis: Structural differences can influence how diseases appear on imaging. Disease Management: Conditions like asthma or COPD may affect each lung differently. Emergency Care: Knowing that aspiration often occurs in the right lung helps guide quick interventions. A qualified Pulmonologist in Guntur uses this anatomical knowledge to provide precise and effective care, especially in cases involving chronic respiratory conditions or congenital anomalies. Summary Your lungs are a perfect example of how the human body values function over symmetry. The right lung is larger and more powerful, while the left lung adapts to accommodate the heart. Together, they create a balanced system that ensures efficient breathing. By understanding lung asymmetry explained, patients and healthcare providers can better recognize potential risks, interpret symptoms accurately, and make informed decisions about respiratory health.
How Big Is Lung Surface Area? The Hidden “Tennis Court” Inside Your Chest
How Big Is Lung Surface Area? The Hidden “Tennis Court” Inside Your Chest The Hidden “Real Estate” Inside Your Chest How big is lung surface area? It sounds unbelievable, but your lungs contain a surface area comparable to a tennis court. Packed within your ribcage is an incredibly efficient biological design that allows you to breathe, move, and live. If all the tiny air sacs in your lungs were spread flat, they would cover roughly 50 to 75 square meters. That’s about the size of a small apartment—compressed into an organ no larger than a pair of grapefruits. This massive surface area is what powers every breath you take. What Are Alveoli? At the ends of your respiratory system lie microscopic structures called alveoli. These are the true workhorses behind breathing. Quantity: Around 480 million alveoli in the human lungs Function: Primary site of oxygen and carbon dioxide exchange Structure: Ultra-thin walls—just one cell thick—for rapid diffusion Think of alveoli as tiny balloons clustered together. Each one increases the total surface area, making gas exchange incredibly efficient. How Big Is Lung Surface Area—and Why Does It Matter? In biology, surface area equals efficiency. The larger the surface, the more space there is for oxygen to enter your bloodstream and carbon dioxide to exit. Here’s a quick breakdown: Feature Lung Specification Total Surface Area 50 – 75 square meters Primary Goal Rapid gas exchange Oxygen Intake Diffusion into blood Waste Removal Carbon dioxide elimination Because of this vast surface, your lungs can handle everything from intense exercise to restful sleep without missing a beat. The “Tennis Court” Comparison Explained To better understand how big lung surface area is, let’s visualize it: Singles tennis court: ~195 square meters Your lungs: ~50–75 square meters Comparison: About 1/3 to 1/2 of a tennis court Now imagine folding that much surface area into your chest. This compact design is one of the most remarkable feats of natural engineering. Why Surface Area Is Critical for Survival Your body constantly needs oxygen to fuel vital organs like the brain, heart, and muscles. The large lung surface area ensures: Maximum oxygen absorption Efficient carbon dioxide removal Stable energy production Without this expansive surface, even simple activities like walking or thinking would become difficult. What Happens When Lung Surface Area Decreases? Damage to alveoli reduces lung surface area, directly impacting your breathing efficiency. Conditions like emphysema cause alveoli to: Lose their shape Merge into larger, less efficient sacs Reduce total surface area This makes oxygen exchange slower and less effective, leading to breathlessness and fatigue. A chest specialist in Guntur often sees patients with reduced lung capacity due to smoking, pollution, or untreated respiratory conditions. How to Protect Your Lung Surface Area Since your lung efficiency depends on maintaining this delicate structure, protecting your alveoli is essential. 1. Avoid Air Pollutants Smoke, dust, and industrial pollution can inflame and damage alveoli. 2. Practice Deep Breathing Deep breathing exercises help expand the lower parts of your lungs, ensuring full utilization of available surface area. 3. Stay Hydrated A thin fluid layer inside alveoli helps gases dissolve and diffuse efficiently. 4. Get Regular Checkups Consulting a chest specialist in Guntur can help detect early signs of lung damage and prevent long-term complications. The Bottom Line So, how big is lung surface area? Surprisingly, it’s as large as a tennis court, folded neatly inside your chest. This enormous surface area is what allows your body to function smoothly every second of the day. Your lungs aren’t just organs—they’re a finely tuned, high-efficiency system designed for survival. The next time you take a deep breath, remember: you’re using a structure as vast as an apartment and as efficient as a high-tech filter—all working silently to keep you alive.
How Fast Is a Sneeze? The Jet-Engine Physics Behind Your Lungs
How Fast Is a Sneeze? The Jet-Engine Physics Behind Your Lungs Ever wondered how fast is a sneeze or why a simple cough can echo across a quiet room? What feels like a small reflex is actually a powerful, high-speed biological defense system. Your lungs, airways, and muscles work together like a precision-engineered pressure chamber—capable of producing explosive bursts of air in milliseconds. Let’s break down the science behind these everyday phenomena and why they matter for your respiratory health. The Anatomy of a Cough: Controlled Power at 50 MPH A cough isn’t random—it’s a highly coordinated mechanism designed to clear your airways. Here’s how it works: Inspiration: You take a deep breath, filling your lungs with air. Compression: Your vocal cords close while chest and abdominal muscles contract, building intense internal pressure. Expulsion: The vocal cords suddenly open, releasing a rapid burst of air. Speed Check:A strong cough can reach speeds of up to 50 miles per hour (80 km/h). This force helps dislodge mucus, dust, or irritants stuck in your respiratory tract. Without this velocity, your lungs would struggle to stay clear. How Fast Is a Sneeze? The 100 MPH Phenomenon Now to the main question: how fast is a sneeze? A sneeze is even more powerful than a cough. It’s your body’s way of clearing the nasal passages—essentially rebooting your air filtration system. Key Facts: Speed: Up to 100 miles per hour (160 km/h) Droplets released: Up to 40,000 microscopic particles Trigger: Irritation in the nasal lining (dust, pollen, viruses) Because your nasal passages are narrower than your throat, the same pressure generates a much higher exit velocity. That’s why sneezes feel more explosive and harder to control. Cough vs. Sneeze: What’s the Difference? Feature Cough Sneeze Speed ~50 mph (80 km/h) ~100 mph (160 km/h) Trigger Area Lower airways Nasal passages Purpose Clear lungs and throat Clean nasal cavity Muscle Action Diaphragm + abdominals Full thoracic compression Both are essential—but they target different parts of your respiratory system. Why Does Speed Matter? These high velocities aren’t just impressive—they’re necessary for survival. 1. Shear Force for Clearing Mucus Thick mucus and debris stick to airway walls. Fast-moving air creates enough force to pull them loose and carry them out. 2. Preventing Deeper Infection Without sufficient speed, irritants could move deeper into your lungs instead of being expelled—potentially causing infections or inflammation. 3. Efficient Airway Reset A sneeze acts like a system reset, clearing allergens and pathogens before they cause harm. The Health Perspective: When to Pay Attention While occasional coughing or sneezing is normal, frequent or severe symptoms may indicate underlying issues. You should consider consulting a Pulmonologist in Guntur if you experience: Persistent cough lasting more than 2–3 weeks Chronic sneezing or nasal irritation Shortness of breath Wheezing or chest tightness A respiratory specialist can assess lung function and identify conditions like asthma, allergies, or infections early. Respiratory Hygiene: Why Covering Matters Given that a sneeze can travel at 100 mph, it’s not just about speed—it’s also about spread. Those thousands of droplets can carry viruses and bacteria across several feet in seconds. Best practices: Cover your mouth and nose with a tissue or elbow Wash hands immediately afterward Avoid close contact when symptomatic This simple hygiene can significantly reduce transmission of respiratory illnesses. The Takeaway So, how fast is a sneeze? Up to 100 miles per hour—making it one of the fastest natural processes your body can produce. Your lungs aren’t just for breathing—they’re dynamic equipped with high-speed defense mechanisms. From a 50 mph cough to a 100 mph sneeze, your body is constantly working to keep your airways clear and healthy. The next time you feel a sneeze coming, remember—you’re witnessing a powerful burst of biological engineering in action. Just make sure you cover up—because at that speed, it’s not something you want to share with the room.
Daily Breathing Capacity of Lungs in Liters: What Your Lungs Do for You Every Day
Daily Breathing Capacity of Lungs in Liters: What Your Lungs Do for You Every Day By Dr. S. Teja, Chest Specialist in Guntur Have you ever paused to think about how much work your lungs do every single day? While many of us focus on steps walked or calories burned, we rarely consider the daily breathing capacity of lungs in liters—a powerful indicator of how hard your respiratory system works to keep you alive. As a practicing chest specialist in Guntur, I often explain to my patients that understanding your breathing is the first step toward protecting your lung health. At Teja Poly Clinic, we see how vital each breath is—not just for survival, but for overall well-being. The Science Behind Your Daily Breathing Capacity An average adult at rest takes about 12 to 20 breaths per minute. This may sound minimal, but when you calculate it over an entire day, the numbers become remarkable. 1. Total Breaths Per Day In 24 hours, you take approximately 20,000 to 22,000 breaths. Your lungs are continuously working—without breaks—to deliver oxygen to your bloodstream and remove carbon dioxide. 2. Daily Breathing Capacity of Lungs in Liters The most fascinating aspect is the total volume of air processed. On average, your lungs handle around 8,000 to 9,000 liters of air per day. This is equivalent to roughly 2,000 to 2,500 gallons. To simplify: That’s enough air to fill a small swimming pool Your lungs function like high-efficiency filters operating 24/7 This enormous daily breathing capacity of lungs in liters highlights just how essential lung care is. Why This Matters for Your Health Because your lungs process such a large volume of air daily, they are constantly exposed to environmental elements such as: Dust and allergens Air pollution Harmful microbes and viruses In cities like Guntur, where air quality can fluctuate, this exposure becomes even more significant. Even small amounts of pollutants, when multiplied by 9,000 liters of air intake daily, can have a noticeable impact on your respiratory health. Common issues that may arise include: Persistent cough or wheezing Shortness of breath Worsening of asthma or COPD Increased risk of respiratory infections As a chest specialist in Guntur, I frequently see patients who ignore early symptoms, not realizing the stress their lungs endure daily. How to Support Your Lung Function Considering the high daily breathing capacity of lungs in liters, taking proactive steps to protect your lungs is crucial. 1. Stay Hydrated Proper hydration helps maintain the mucosal lining of your lungs, allowing them to trap and remove harmful particles effectively. 2. Limit Exposure to Pollution On days with poor air quality, reduce outdoor activities. Wearing a mask can also minimize inhalation of harmful pollutants. 3. Exercise Regularly Physical activity improves lung efficiency and capacity. Even simple exercises like walking or breathing techniques can enhance oxygen intake. 4. Avoid Smoking and Passive Smoke Smoking significantly damages lung tissues and reduces their filtering ability. Avoid both active and passive exposure. 5. Schedule Regular Check-Ups If you experience symptoms like chronic cough, chest tightness, or breathlessness, consult a professional without delay. Early diagnosis can prevent serious complications. When Should You See a Specialist? Your lungs may be silently struggling even before symptoms become severe. If you notice: Frequent respiratory infections Reduced stamina Difficulty breathing during routine activities It’s time to consult a qualified expert. As a trusted chest specialist in Guntur, I emphasize early intervention to maintain optimal lung health. Prioritize Your Breathing, Prioritize Your Life Your lungs process thousands of liters of air every day—often without you even noticing. This incredible system deserves attention and care. Understanding the daily breathing capacity of lungs in liters is not just a fascinating fact; it’s a reminder of how essential lung health is to your overall quality of life. At Teja Poly Clinic, Guntur, we are committed to helping you breathe better and live healthier. Take a moment today to appreciate your lungs—and take the necessary steps to protect them. Your lungs work tirelessly for you. Make sure you return the favour.
The Invisible Storm: Thunderstorm Asthma Symptoms and Prevention
The Invisible Storm: Thunderstorm Asthma Symptoms and Prevention Summer is often associated with sunshine, vacations, and outdoor fun—but it also brings hidden health risks. One of the most overlooked dangers is thunderstorm asthma, a rare yet serious condition that can trigger sudden breathing difficulties. While storms may seem refreshing, they can turn dangerous for people with allergies, hay fever, or asthma. Understanding thunderstorm asthma symptoms and prevention is essential, especially during peak pollen seasons, to protect your respiratory health. What is Thunderstorm Asthma? Thunderstorm asthma occurs when specific weather conditions during a storm interact with airborne pollen, transforming it into a respiratory hazard. Normally, pollen grains are too large to enter the lungs deeply. They get trapped in the nose or throat, causing common hay fever symptoms like sneezing and itching. However, during a thunderstorm, the situation changes dramatically: Moisture Absorption: High humidity before a storm causes pollen grains to absorb water and swell. Pollen Rupture: These swollen grains burst into hundreds of tiny fragments. Wind Distribution: Strong storm winds push these microscopic particles toward ground level. Deep Lung Inhalation: The tiny particles bypass natural nasal filters and travel deep into the lungs. This chain reaction increases the risk of asthma attack triggers, even in people who may not have been previously diagnosed with asthma. Thunderstorm Asthma Symptoms to Watch For Recognizing thunderstorm asthma symptoms early can be life-saving. Symptoms often develop quickly and can worsen within minutes. Common warning signs include: Sudden shortness of breath Tightness or pressure in the chest Persistent coughing Wheezing or whistling sounds while breathing Difficulty speaking in full sentences If these symptoms appear during or just before a storm, seek medical attention immediately. Thunderstorm asthma can escalate rapidly and requires urgent care. Who is Most at Risk? You don’t need a history of asthma to be affected. However, certain individuals are more vulnerable: 1. People with Seasonal Hay Fever Those suffering from pollen allergy or allergic rhinitis—especially due to grass pollen—are at higher risk. 2. Individuals with Undiagnosed Asthma People who experience occasional wheezing, coughing, or breathlessness during summer may unknowingly have asthma. 3. People with Existing Asthma Those with poorly controlled asthma or irregular use of preventer medications are particularly at risk during storms. Understanding your personal risk is a key step in effective thunderstorm asthma prevention. Thunderstorm Asthma Prevention: How to Stay Safe Taking proactive steps can significantly reduce your risk. Here are practical and effective thunderstorm asthma prevention tips: 1. Monitor Weather and Pollen Forecasts Keep an eye on daily pollen levels and thunderstorm warnings. Many weather apps now provide pollen alerts, helping you plan ahead. 2. Stay Indoors During Storms When a storm is approaching: Close all windows and doors Avoid outdoor exposure Set your air conditioner to “recirculate” mode This helps limit exposure to airborne allergens. 3. Avoid the Storm Front The highest risk period is just before rainfall begins, when strong winds carry pollen particles at ground level. Avoid stepping outside during this time. 4. Keep Your Medication Ready Always carry your reliever inhaler and ensure it is within expiry. If you have asthma, follow your prescribed treatment plan strictly. 5. Consult Your Doctor If you experience severe summer allergies or hay fever, discuss a preventive asthma management plan with your healthcare provider before the season peaks. Why Awareness Matters Thunderstorm asthma events can affect large groups of people at once, overwhelming healthcare systems. Increasing awareness about thunderstorm asthma symptoms and prevention can help individuals act quickly and reduce complications. Final Thoughts Thunderstorms may bring cooler temperatures, but they can also trigger a dangerous mix of airborne allergens. By understanding how thunderstorm asthma works and recognizing its symptoms early, you can take control of your respiratory health. Stay informed, stay prepared, and prioritize prevention—because when it comes to respiratory health, awareness is your strongest defence against the invisible storm.
AC Trap Health Risks Explained by a Pulmonologist in Guntur
AC Trap Health Risks Explained by a Pulmonologist in Guntur As a pulmonologist in Guntur with over 10 years of clinical experience, I often see a surge in patients during peak summer—not because of infections alone, but due to something far more overlooked: the AC trap. While air conditioning offers much-needed relief from scorching temperatures, improper use can quietly trigger a range of respiratory issues. Let’s break down the AC trap health risks explained in a clear, practical way so you can stay cool without compromising your health. What Is the “AC Trap”? The AC trap refers to the chain reaction your body undergoes when exposed to sudden temperature changes and poorly maintained air conditioning systems. It’s not a disease—but it can mimic one, causing symptoms like: Sneezing Throat irritation Nasal congestion Dry cough Headache and fatigue Many patients assume it’s a viral infection, but in reality, it’s often a response to environmental stress. 1. Thermal Shock: The Hidden Stress on Your Airways When you move from 40°C outdoor heat to a 20–22°C indoor environment, your respiratory system struggles to adapt quickly. What happens inside your body? Airway constriction: Cold air causes bronchial muscles to tighten, especially in people with asthma or allergies. Dryness and irritation: AC air lacks humidity, drying out your throat and nasal lining. Excess mucus production: Your body tries to protect itself, leading to a blocked or runny nose. As a pulmonologist in Guntur, I frequently see patients with worsening asthma symptoms triggered purely by this sudden thermal shift. 2. Indoor Air Quality: The “Invisible Guests” in AC Systems Another major part of AC trap health risks explained is poor maintenance of cooling systems. If your AC hasn’t been cleaned regularly, it may circulate more than just cool air. Common contaminants include: Mold and fungi: Thrive in damp coils and ducts Dust and pollen: Accumulate in clogged filters Bacteria: Grow in stagnant water inside the unit These particles are continuously blown into your breathing space, leading to: Allergic rhinitis Sinus irritation Bronchial inflammation Increased risk of respiratory infections In my clinical practice, I’ve seen patients improve dramatically simply by servicing their AC units. 3. Who Is Most at Risk? While anyone can fall into the AC trap, certain groups are more vulnerable: Children Elderly individuals People with asthma or COPD Those with frequent allergies Office workers exposed to AC for long hours If you belong to any of these groups, extra precautions are essential. How to Avoid the AC Trap (Practical Tips) You don’t need to give up your AC—just use it wisely. 1. Follow the “Buffer Zone” Method Before entering a fully air-conditioned space, spend a few minutes in a shaded or fan-cooled area. This helps your body adjust gradually. 2. Maintain Your AC Regularly Clean filters every 30–90 days Schedule professional servicing periodically Ensure proper drainage to avoid bacterial buildup 3. Control Humidity AC units dry the air significantly. To prevent throat irritation: Use a humidifier Stay well hydrated Keep indoor plants or a bowl of water nearby 4. Follow the Temperature Gap Rule Avoid extreme contrasts. Ideally: Keep indoor temperature 8–10°C lower than outdoor temperature Avoid setting AC below 22°C for prolonged periods 5. Protect Your Airways Drink warm water regularly Avoid direct airflow on your face or chest Use a light scarf if exposed for long durations When Should You See a Pulmonologist? If symptoms persist beyond a few days or worsen, consult a specialist. Warning signs include: Continuous cough Wheezing or breathlessness Recurrent throat infections Severe nasal blockage Early evaluation can prevent minor irritation from becoming a chronic respiratory issue. The Bottom Line The AC trap health risks explained are not meant to scare you—but to help you make smarter choices. Air conditioning is essential in cities like Guntur, where summer temperatures are extreme. However, balancing comfort with health is key. As a Pulmonologist in Guntur, my advice is simple:Respect the transition, maintain your environment, and listen to your body. Stay cool—but stay healthy too.
Sticky Mucus in Summer Causes: Why 40°C Heat Affects Your Airways (Expert Insights from a Pulmonologist)
Sticky Mucus in Summer Causes: Why 40°C Heat Affects Your Airways (Expert Insights from a Pulmonologist) When temperatures soar to 40°C, your body works overtime to maintain balance. While most people focus on heatstroke or dehydration, there’s a lesser-known issue affecting your respiratory system—sticky mucus in summer. As a pulmonologist with over 10 years of experience, I often see patients complaining of a “gunky throat,” persistent coughing, or chest congestion during peak summer. Many assume it’s an infection, but in reality, the root cause is often heat-induced dehydration affecting your airway function. Understanding the sticky mucus in summer causes can help you protect your respiratory health and breathe more comfortably during extreme heat. The Science Behind Sticky Mucus in Summer Your respiratory tract is naturally lined with a thin, watery layer of mucus. This mucus plays a critical role—it traps dust, allergens, and microbes while tiny hair-like structures called cilia move it out of your system. However, during extreme heat, this system begins to fail. 1. Dehydration and Water RedistributionAt 40°C, your body prioritizes hydration for vital organs like the brain and heart. As a result, less water is available for your airway lining. This leads to dryness in your throat and lungs. 2. Thickening of MucusOne of the primary sticky mucus in summer causes is the loss of moisture. When mucus loses water, it becomes thick, sticky, and difficult to move—more like glue than a protective fluid. 3. Cilia DysfunctionCilia depend on a watery environment to function effectively. When mucus thickens, these tiny structures slow down or stop working, allowing mucus to accumulate instead of being cleared. 4. Airway Blockage and IrritationInstead of flushing out irritants, thick mucus traps them inside your airways. This results in congestion, coughing, throat irritation, and sometimes breathlessness. Health Risks of Sticky Mucus in Summer Sticky mucus isn’t just uncomfortable—it can lead to serious respiratory concerns, especially during heatwaves. Increased IrritationPollutants, dust, and pollen remain trapped longer in thick mucus, causing continuous irritation. Higher Risk of InfectionsBacteria and viruses thrive in stagnant mucus. This increases the chances of respiratory infections. Worsening of Chronic ConditionsPatients with asthma, bronchitis, or COPD are particularly vulnerable. Thick mucus can trigger flare-ups and breathing difficulties. If symptoms persist, consulting the Best Pulmonologist in Guntur can help diagnose and manage the condition effectively. Sticky Mucus in Summer Causes: Key Triggers To summarize, the main causes include: Dehydration due to excessive heat Reduced fluid intake High caffeine consumption Exposure to dry air and pollutants Underlying respiratory conditions How to Prevent Sticky Mucus in Summer Managing sticky mucus in hot weather is simple if you take the right steps. Here are three clinically recommended strategies: 1. Stay Hyper-HydratedHydration is the most effective solution. Drinking adequate water helps maintain mucus in its thin, slippery form, allowing your body to clear it naturally. Aim for at least 3–4 liters of water daily in extreme heat Include hydrating foods like watermelon, cucumber, and coconut water 2. Use Nasal Saline SpraysSaline sprays help rehydrate your nasal passages and upper airway lining. This is especially useful if you spend time in air-conditioned environments, which can dry out your airways. 3. Limit Excess Caffeine IntakeWhile moderate coffee consumption is fine, excessive caffeine can act as a diuretic, increasing fluid loss and worsening dehydration. When to See a Specialist If you experience persistent symptoms such as: Continuous chest congestion Thick phlegm that doesn’t clear Difficulty breathing Frequent coughing It’s important to seek medical advice. Consulting the Best Pulmonologist in Guntur ensures proper evaluation and timely treatment. Conclusion Sticky mucus in summer is a direct result of dehydration and extreme heat stress on your body. While it may seem minor, it can significantly impact your respiratory health if ignored. The key takeaway is simple: hydration is not just about thirst—it’s essential for keeping your airways clear and functioning properly. By understanding the sticky mucus in summer causes and taking preventive measures, you can stay comfortable, healthy, and breathe easily—even in 40°C heat.
The Invisible Weight: How Humidity Worsens Asthma Symptoms (Expert Insights from an Asthma Specialist in Guntur)
The Invisible Weight: How Humidity Worsens Asthma Symptoms (Expert Insights from an Asthma Specialist in Guntur) If you’ve ever stepped outside on a muggy day and felt like the air was “too heavy” to breathe, you’re not alone. As a pulmonologist with over a decade of experience, I’ve consistently observed how humidity worsens asthma symptoms in many patients. What may feel like mild discomfort for others can become a serious respiratory challenge for individuals with asthma. Let’s understand why this happens and how you can protect your lungs. Why Humidity Worsens Asthma Symptoms High humidity means there is excessive moisture in the air. This creates an environment that puts extra strain on already sensitive airways. 1. “Heavy Air” Increases Breathing Effort Humid air often feels thicker, making it harder to breathe. When humidity worsens asthma symptoms, patients commonly experience: Shortness of breath Chest tightness Fatigue while breathing This happens because your respiratory muscles must work harder to move moist air in and out of the lungs. 2. Triggers Bronchospasms Warm, damp air can irritate airway nerves, leading to bronchospasms—a sudden narrowing of the airways. This is one of the main reasons humidity worsens asthma symptoms, causing: Wheezing Persistent coughing Sudden breathing difficulty These flare-ups can occur quickly, especially during hot and humid weather. Hidden Triggers: Dust Mites and Mold Another major reason humidity worsens asthma symptoms is the increase in indoor allergens. Dust Mites Dust mites thrive in humidity levels above 50%. They absorb moisture from the air and multiply rapidly. Their waste particles: Are microscopic Easily inhaled Cause airway inflammation This leads to continuous irritation and worsening asthma control. Mold Growth High humidity promotes mold growth in damp areas such as: Bathrooms Kitchens Walls and carpets Mold releases airborne spores that can trigger severe asthma symptoms, including sudden attacks. Common Signs That Humidity Worsens Asthma Symptoms You may notice your asthma getting worse during rainy or humid days. Key warning signs include: Increased wheezing Frequent coughing (especially at night) Tightness in the chest Reduced ability to exercise Increased reliance on inhalers If these symptoms persist, consulting an expert like an Guntur-based Asthma Specialist is highly recommended. How to Reduce the Impact of Humidity While you can’t control outdoor weather, you can manage your indoor environment effectively. 1. Maintain Ideal Humidity Levels Keep indoor humidity between 30% and 45% using a hygrometer. 2. Use a Dehumidifier A dehumidifier helps remove excess moisture, especially in: Basements Coastal or humid regions This is one of the most effective ways to prevent triggers. 3. Improve Ventilation Always use exhaust fans: While cooking During showers This prevents moisture buildup indoors. 4. Clean Smartly Use a damp cloth instead of dry dusting to trap allergens rather than spreading them in humid air. 5. Use Air Conditioning Air conditioners help regulate both temperature and humidity. On humid days: Keep windows closed Run your AC to maintain dry, breathable air When to See an Asthma Specialist in Guntur If humidity worsens asthma symptoms frequently or your condition is not well-controlled, it’s important to seek medical advice. A qualified Asthma Specialist in Guntur can: Adjust your treatment plan Identify triggers Improve long-term asthma control The Bottom Line There is a clear and direct link between environmental conditions and respiratory health. Simply put, humidity worsens asthma symptoms by making breathing harder and increasing exposure to allergens like dust mites and mold. By controlling indoor humidity and staying alert to early symptoms, you can significantly improve your breathing and overall quality of life. Quick Question:Do you monitor humidity levels at home, or do you rely on how the air feels?
Can Hot Air Cause Bronchospasm? The Hidden Danger You Shouldn’t Ignore
Can Hot Air Cause Bronchospasm? The Hidden Danger You Shouldn’t Ignore Have you ever stepped into scorching heat and suddenly felt your chest tighten, as if your breath was being taken away? It’s a frightening sensation—one that many people dismiss as “just the heat.” But the truth is more serious. Can hot air cause bronchospasm? Yes, it absolutely can—and for some, it can be dangerous. We often associate breathing problems with cold air, especially in winter or during exercise. But extreme heat can be just as harsh on your lungs, silently triggering reactions that many don’t expect. What Happens When You Inhale Hot Air? Your lungs are delicate. They are designed to function best at a stable internal temperature. When you inhale air that is significantly hotter than your body temperature, it doesn’t just feel uncomfortable—it can act like an invisible irritant. A bronchospasm occurs when the muscles around your airways suddenly tighten. This narrowing makes it difficult for air to move in and out of your lungs. When hot air enters your respiratory system, it can trigger this exact response—almost instantly. Can Hot Air Cause Bronchospasm? Here’s Why The answer lies in how your body tries to protect itself. 1. Thermal Irritation Think about how your skin reacts to heat. Now imagine that same effect happening inside your airways. Hot air can irritate the lining of your lungs, causing them to constrict as a defense mechanism. 2. Inflammatory Response High temperatures can stimulate your body to release chemicals like histamines. These chemicals lead to swelling and tightening of the airways, making breathing harder. 3. Humidity Overload Hot air is often heavy with moisture. This thick, humid air can feel suffocating and harder to process, especially if your lungs are already sensitive. Symptoms You Should Never Ignore If you’ve been exposed to extreme heat and notice any of the following symptoms, your body may be reacting to hot air inhalation: Tightness or pressure in the chest Sudden wheezing or whistling sounds while breathing Shortness of breath (dyspnea) Persistent dry cough after exposure These symptoms can appear within minutes. For someone with asthma or other respiratory conditions, they can escalate quickly. Who Is Most at Risk? While anyone can be affected, certain groups need to be especially careful: People with asthma Individuals with COPD Those exposed to industrial heat or fire environments People living in extremely hot and humid climates If you fall into one of these categories, your lungs may react more aggressively to heat exposure. How to Protect Your Lungs from Heat The good news is that simple precautions can make a big difference. Stay Hydrated Water helps maintain the moisture balance in your airways, making them less reactive to heat. Breathe Through Your Nose Your nose acts like a natural filter and temperature regulator. It slightly cools the air before it reaches your lungs. Avoid Peak Heat Limit outdoor activities when temperatures rise above normal body temperature (around 37°C). Early mornings or evenings are safer. Keep Medication Ready If you have asthma or a history of bronchospasm, always carry your rescue inhaler. Heat is a real trigger—don’t underestimate it. A Gentle Reminder for Your Health So, can hot air cause bronchospasm? Yes—and often faster than you expect. Your lungs are incredibly sensitive, and when exposed to extreme heat, they react instinctively to protect you. But that protection can feel like panic—like your breath is slipping away. Listening to your body is essential. That tightness in your chest, that sudden breathlessness—it’s not something to ignore. If you frequently experience these symptoms, consider consulting a specialist. A trusted pulmonologist can help you understand your triggers and guide you toward safer breathing, even in challenging climates. Final Thought Breathing is something we take for granted—until it becomes difficult. Heat may seem harmless, even comforting at times, but for your lungs, it can be a silent stressor. Stay aware. Stay cool. And most importantly—protect every breath you take.
Eosinophilia Symptoms and Treatment: 7 Key Clinical Insights You Should Know
Eosinophilia Symptoms and Treatment: 7 Key Clinical Insights You Should Know Eosinophilia Symptoms and Treatment Eosinophilia is not just a lab abnormality—it is a complex immune response that can significantly impact lung health and overall well-being. Understanding Eosinophilia Symptoms and Treatment is essential for both patients and healthcare providers, especially when dealing with respiratory conditions like Eosinophilic Asthma and pulmonary disorders. Below are 7 important clinical insights that highlight how eosinophils affect the body, along with key symptoms and treatment approaches. 1. Why Eosinophils Overreact (Hygiene Hypothesis) Eosinophils are specialized white blood cells designed to fight parasites. However, in today’s cleaner environments, these cells often lack real threats. As a result, they may overreact to harmless triggers like dust, pollen, or allergens. This leads to common Pulmonary Eosinophilia Symptoms such as: Wheezing Shortness of breath Chronic cough Proper diagnosis is crucial to avoid mistaking this condition for regular asthma. 2. Lung Damage and Airway Remodeling In conditions like Eosinophilic Asthma, eosinophils release toxic proteins that damage airway tissues. Over time, this can cause permanent structural changes known as airway remodeling. Symptoms include: Persistent breathing difficulty Reduced lung function Frequent asthma attacks Treatment:Early intervention with corticosteroids or biologic therapies is key to preventing irreversible damage. 3. Pulmonary Eosinophilia Caused by Parasites Certain parasitic infections can lead to pulmonary eosinophilia when larvae migrate through the lungs. Pulmonary Eosinophilia Symptoms: Dry cough Fever Chest discomfort Temporary lung infiltrates on imaging Treatment:Anti-parasitic medications combined with supportive care effectively resolve symptoms. 4. Crystal Formation in Airways Eosinophils can break down and form microscopic crystals in the airways, indicating severe inflammation. Symptoms: Thick mucus production Severe coughing Breathing obstruction Treatment:Managing inflammation with steroids and controlling triggers is essential for relief. 5. EGPA Symptoms Can Mimic Asthma Eosinophilic Granulomatosis with Polyangiitis (EGPA) often begins as adult-onset asthma but progresses into a serious condition affecting multiple organs. EGPA Symptoms include: Severe asthma Sinusitis Skin rashes Nerve pain or numbness Fatigue Treatment:Immunosuppressants and corticosteroids are required to control inflammation and prevent organ damage. 6. Recognizing Eosinophilia Symptoms Early Common Eosinophilia Symptoms may vary depending on the affected organ but often include: Persistent cough and wheezing Breathlessness Skin rashes or itching Fatigue Fever in some cases Early recognition plays a vital role in effective treatment and prevention of complications. 7. Drug-Induced Eosinophilia Certain medications can trigger eosinophilic lung reactions, leading to inflammation that mimics pneumonia. Common triggers: Antibiotics Pain relievers (NSAIDs) Anti-seizure medications Symptoms: Sudden breathlessness Fever Lung infiltrates Treatment:Stopping the offending drug and starting corticosteroids usually leads to rapid recovery. Eosinophilia Treatment Options Managing Eosinophilia Symptoms and Treatment depends on the underlying cause. Common treatment approaches include: Corticosteroids: Reduce inflammation quickly Biologic therapies: Target specific immune pathways in severe cases Anti-parasitic drugs: For infection-related eosinophilia Avoiding triggers: Allergens or medications Regular monitoring: Blood tests and lung function tests For patients experiencing persistent respiratory symptoms, consulting an expert is essential. If you are in Andhra Pradesh, consider visiting an experienced Asthma Specialist in Guntur for accurate diagnosis and personalized treatment. Key Takeaways Understanding Eosinophilia Symptoms and Treatment is critical for preventing long-term complications like lung damage and organ involvement. Conditions such as Eosinophilic Asthma and EGPA can often be misdiagnosed, delaying proper care. If your asthma symptoms are not improving with standard inhalers, it may be time to investigate underlying eosinophilia. Early diagnosis, targeted treatment, and expert consultation can significantly improve quality of life and prevent serious health risks.
Drug Caused Eosinophilic Pneumonia Symptoms: The Hidden Cause Behind Severe “Pneumonia”
Drug Caused Eosinophilic Pneumonia Symptoms: The Hidden Cause Behind Severe “Pneumonia” It often begins like a typical chest infection. A dry cough, rising fever, and breathlessness make it seem like pneumonia. Even the chest X-ray shows cloudy patches that strongly suggest infection. However, in some cases, the real culprit is not bacteria or viruses—it is the medication itself. This condition is known as Drug Caused Eosinophilic Pneumonia, a rare but serious reaction that can rapidly worsen if not identified early. Understanding drug caused eosinophilic pneumonia symptoms is crucial because early recognition can prevent complications and save lives. What is Drug Caused Eosinophilic Pneumonia? Drug Caused Eosinophilic Pneumonia occurs when the body’s immune system reacts abnormally to certain medications. Instead of fighting infection, white blood cells called eosinophils accumulate in the lungs, causing inflammation and fluid buildup. This disrupts oxygen exchange and leads to severe respiratory distress. The condition can develop within days or weeks after starting a new medication, often without any prior warning. Drug Caused Eosinophilic Pneumonia Symptoms to Watch For The biggest challenge with this condition is that its symptoms closely mimic common respiratory infections. Key drug caused eosinophilic pneumonia symptoms include: Persistent dry cough High fever and chills Sudden shortness of breath Chest discomfort or tightness Night sweats and fatigue Worsening breathing despite antibiotics These symptoms can escalate quickly. If left untreated, patients may develop severe oxygen deficiency requiring hospitalization. Why It Is Often Misdiagnosed Drug Caused Eosinophilic Pneumonia is often called a “medical imposter” because it looks almost identical to bacterial pneumonia: Chest X-rays show infiltrates similar to infection Symptoms overlap with viral or bacterial illness Initial treatment typically involves antibiotics The problem arises when patients do not improve with antibiotics. Since the underlying cause is an immune reaction—not infection—standard treatments fail, and the condition worsens. This is where consulting a Lung Specialist in Guntur becomes critical for accurate diagnosis and timely intervention. Common Medications That Can Trigger the Condition While Drug Caused Eosinophilic Pneumonia is rare, several commonly used medications are known triggers: Antibiotics: Nitrofurantoin, Daptomycin Painkillers (NSAIDs): Ibuprofen, Naproxen, Aspirin Anti-seizure drugs: Phenytoin, Carbamazepine Antidepressants: Venlafaxine, Sertraline Heart medications: Amiodarone These medications are generally safe for most people, but in rare cases, they can trigger a strong eosinophilic response. What Happens Inside the Lungs? In this condition, eosinophils—cells usually involved in allergic reactions—invade the alveoli (tiny air sacs in the lungs). Instead of protecting the body, they release toxic substances that damage lung tissue. This results in: Inflammation of lung tissue Fluid buildup in the air spaces Reduced oxygen levels in the blood As oxygen exchange becomes impaired, patients experience worsening breathlessness and fatigue. Diagnosis: Identifying the Real Cause Accurate diagnosis is essential to avoid unnecessary treatments. A key diagnostic procedure is Bronchoalveolar Lavage (BAL), where fluid is collected from the lungs and analyzed. A high eosinophil count (usually above 25%) strongly indicates eosinophilic pneumonia. An experienced Lung Specialist in Guntur can differentiate this condition from other lung diseases using clinical history, imaging, and lab tests. Treatment: Rapid and Effective Recovery Unlike bacterial pneumonia, Drug Caused Eosinophilic Pneumonia does not respond to antibiotics. The treatment approach includes: Immediate discontinuation of the suspected medication Corticosteroid therapy (such as Prednisone) The response is often dramatic. Many patients show significant improvement within 24 to 48 hours after starting steroids, with rapid clearing of lung inflammation. When Should You Seek Medical Help? If you are being treated for pneumonia but do not improve after 48 hours of antibiotics, it is important to reassess the diagnosis—especially if you recently started a new medication. Early consultation with a Lung Specialist in Guntur can help identify drug caused eosinophilic pneumonia symptoms and ensure timely, life-saving treatment. Final Thoughts Drug Caused Eosinophilic Pneumonia is a rare but serious condition that can easily be mistaken for common infections. Recognizing the symptoms early and understanding the role of medications can make a critical difference. Always inform your doctor about any recent medications and do not ignore persistent respiratory symptoms. Timely diagnosis and expert care are key to protecting your lung health.
Parasite Lung Migration Symptoms: A Simple Guide to Löffler’s Syndrome
Parasite Lung Migration Symptoms: A Simple Guide to Löffler’s Syndrome Imagine having a persistent cough—not from a cold, but from parasites briefly passing through your lungs. This unusual condition is called Löffler’s Syndrome, and it’s closely linked to parasite lung migration symptoms. What is Löffler Syndrome Explained Simply Löffler’s Syndrome is a temporary lung condition where a type of white blood cell called eosinophils builds up in the lungs. This usually happens when parasite larvae migrate through the lungs as part of their life cycle. In simple terms: Parasites enter your body → travel through your bloodstream → pass through your lungs → then settle in your intestines. Why Do Parasites Travel Through Lungs? You might wonder, why do parasites travel through lungs at all? It’s part of their natural life cycle. Parasites like: Ascaris lumbricoides Ancylostoma duodenale Necator americanus Strongyloides stercoralis need the lungs as a transit point to mature properly. The oxygen-rich environment helps them develop before they move to the intestines where they grow into adult worms. How Worms Move from Intestine to Lungs Understanding how worms move from intestine to lungs (or vice versa) helps explain the symptoms: Entry into the body Swallowing contaminated food (roundworms) Skin penetration (hookworms) Bloodstream journey Larvae enter circulation and travel through veins Arrival in lungs They break into tiny air sacs (alveoli) Climbing upward Move up the airways (bronchi → trachea) Return to intestine Coughed up and swallowed back into the digestive tract Parasite Lung Migration Symptoms When parasites pass through the lungs, your immune system reacts strongly. Common parasite lung migration symptoms include: Persistent dry cough Wheezing (similar to asthma) Shortness of breath Mild fever Chest discomfort Temporary lung shadows on X-ray (that appear and disappear) These symptoms are often mistaken for asthma or pneumonia. Diagnosis: How Doctors Identify It Doctors look for clues such as: High eosinophil count in blood tests Larvae in sputum (sometimes) Migrating lung infiltrates on imaging If you’re experiencing these symptoms, consulting a specialist like a Pulmonologist in Guntur can help ensure accurate diagnosis and treatment. Treatment and Recovery The condition usually improves on its own once larvae leave the lungs. However, treatment is important to stop reinfection: Antiparasitic medications (e.g., albendazole) Steroids in severe cases (to reduce inflammation) Prevention Tips To avoid parasite infections: Wash hands thoroughly Clean fruits and vegetables properly Avoid walking barefoot in contaminated soil Maintain good hygiene and sanitation The Bottom Line Parasite lung migration symptoms may sound alarming, but Löffler’s Syndrome is usually temporary and treatable. Knowing why parasites travel through lungs and how worms move from intestine to lungs helps you recognize early signs and seek proper care. If symptoms persist, don’t ignore them—early consultation with a lung specialist can make all the difference.